
Update from CIG Asset Management – What’s Your Benchmark?
Do you compare your investment portfolio’s performance to a popular stock that you hear about on CNBC?
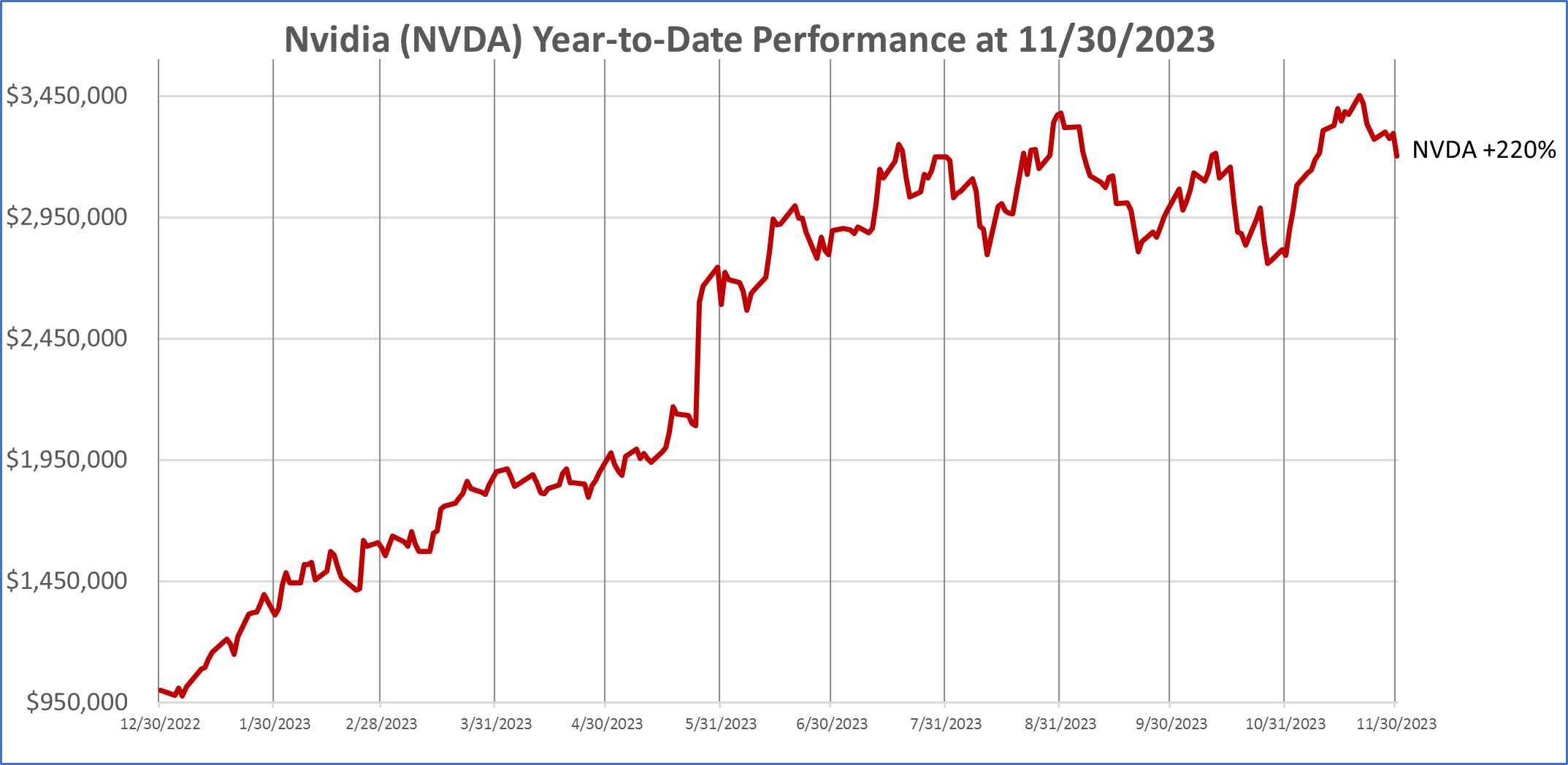
This is the daily chart for Nvidia, a single stock that soared +220% year-to-date through November 30, 2023. [i]
Maybe you compare your portfolio to the S&P 500.
Year-to-date through November 30, 2023, the S&P 500, represented by the SPDR S&P 500 ETF (SPY), is up +20.7%. [ii] It might be appropriate to use the S&P 500 as your benchmark if you invest all your money in large and mid-sized companies that are domiciled in the United States. However, if you are using an important tool like many investors in managing investment risk – diversification – that is, spreading your investments among and within different asset classes, then comparing your performance to the S&P 500 is likely to leave you disappointed.
This year, that disappointment is likely to be WORSE because as we discussed last month in Year-to-Date U.S. Stock Performance in Pictures, the S&P 500 performance thus far this year had been dominated by just 7 stocks – the Magnificent 7 – which Torsten Slok, Chief Economist at Apollo Asset Management said were becoming more and more overvalued and, in our view, more dangerous to invest in. [iii] Are we headed toward a big loss like post the year 2000, when the dot com stocks fell and the S&P 500 had fallen -49% from its peak on March 27, 2000, to its low On October 9, 2022? [iv]
At CIG, we believe in the adage, “Don’t put all your eggs in one basket”. We employ active asset allocation to employ varying levels of exposure to various sectors of domestic and international stocks, fixed income, and alternatives, such as gold and commodities, in an attempt to manage risk throughout market cycles.
How do we compare our strategies’ performance?
At CIG, we utilize benchmarks that are invested in a blend of three major asset classes- domestic equities, international equities, and fixed income.
- Domestic equities are represented by the Russell 3000 Index, a market capitalization-weighted index which measures the performance of the 3,000 largest U.S. companies and representing approximately 96% of the investible U.S. equity market. [v]
- International equities are represented by the MSCI ACWI ex USA Index, an index covering approximately 85% of the global equity opportunity set outside of the United States. [vi]
- Fixed income is represented by the Bloomberg U.S. Aggregate Index, an index composed of investment-grade government and corporate bonds. [vii]
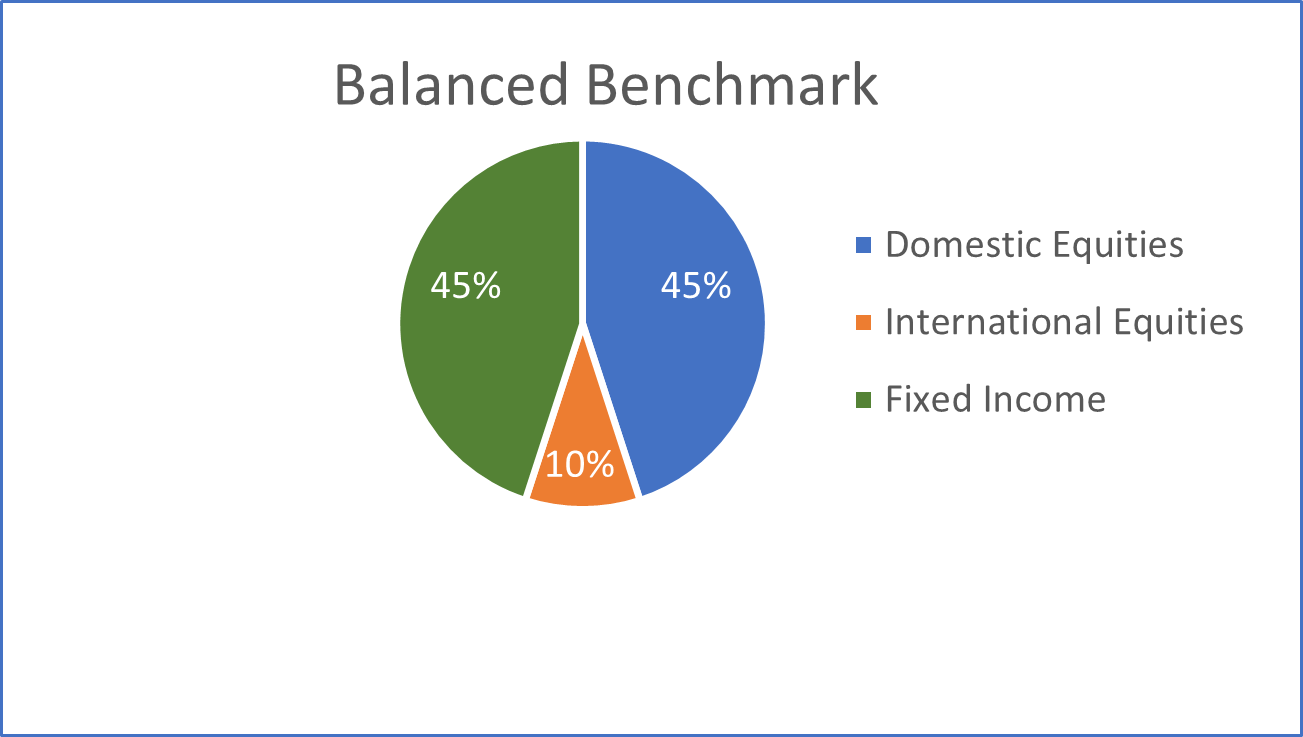
The pie chart below illustrates the weightings of the three major asset classes in our balanced benchmark. We compare the performance of our clients whom we generally describe as balanced investors to the performance of this balanced benchmark.
In the following bar chart, we compare year-to-date performance of the components of our balanced benchmark to the S&P 500 and Equal-Weighted S&P 500 as of November 30, 2023.
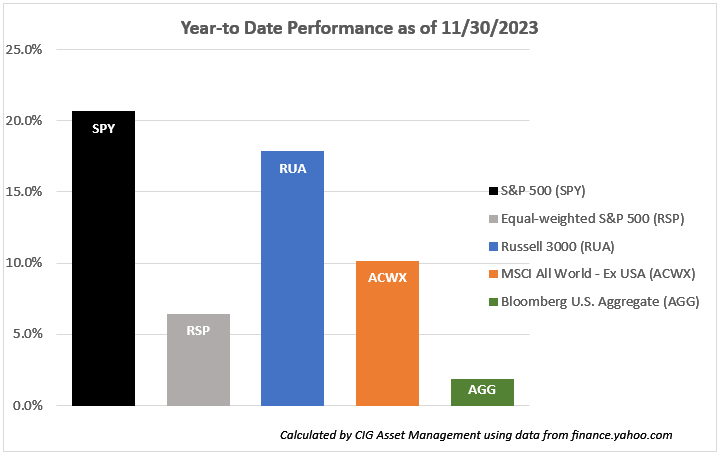
Year-to-date, the Russell 3000 – the domestic equity index we use in our benchmarks – gained +17.8%. The Russell 3000 has a similar issue to Magnificent 7 stock dominance, with 24% of the index invested in these seven stocks but not to the same extent as the S&P 500, with 28%. [viii] Over the same period, the MSCI ACWI ex USA index (ACWX) gained +10.1%, less than half of the S&P 500, and the Bloomberg U.S. Aggregate Index (AGG) was only up +1.9%. [ix] This year, if you employed diversification – spreading your investments among and within different asset classes in the chart above instead of only investing in the S&P 500, you clearly experienced lower returns than the S&P 500.
Now that we have told you about our balanced benchmark, what is the appropriate period to assess how one has done versus the benchmarks? Should you look at it every day? How should we be looking at returns and the amount of risk you are taking?
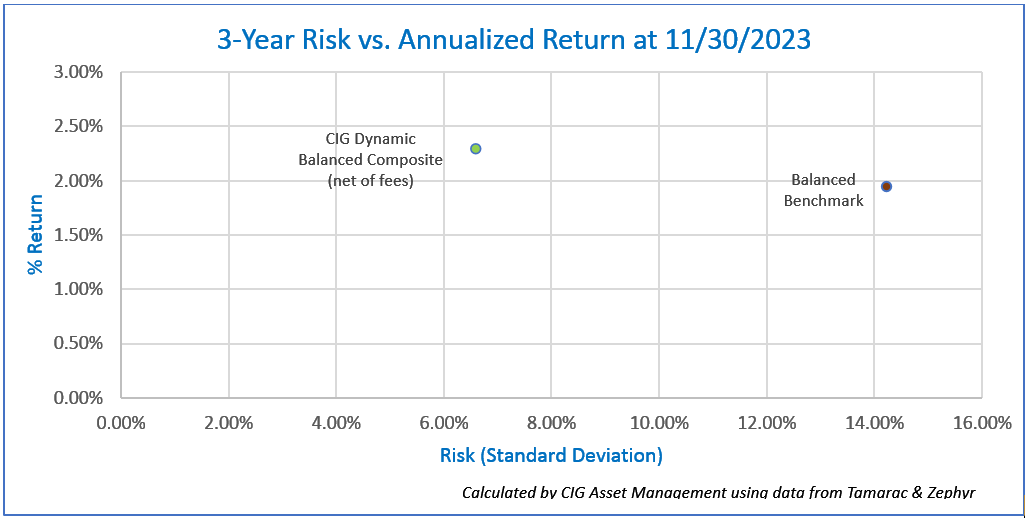
We prefer to look at returns and risk over a trailing 3-year period. We measure risk using the standard deviation of returns. The CIG Dynamic Balanced Composite trailing 3-Year annualized return as of November 30, 2023, is +2.30%, net of fees, and the 3-year standard deviation is 6.6%. [x] The Balanced Benchmark’s trailing 3-year annualized return as of November 30, 2023, is +1.95% and the 3-year standard deviation is 14.2%. [xi]
You can see in the chart below that the CIG Dynamic Balanced Composite is taking less than half (46%) of the risk, as measured by the standard deviation of annualized three year returns, of the balanced benchmark [xii] and is returning 118% of the balanced benchmark’s return on a trailing 3-year annualized basis. [xiii]
At CIG, we believe in risk-balanced investing. We believe investors should consider how much risk they are taking to achieve returns. We think that we should be striving to reach the return necessary to meet the various needs of our client’s financial plans while, at this point in the market cycle, taking as little risk as possible to meet that goal. We want you to sleep at night.
Speaking of risk, let’s go back to the first chart on page one, Nvidia (NVDA). Nvidia has experienced many booms and busts over the years. The stock is currently booming, up +220% year-to-date through November 30, 2023, due to surging sales of its artificial intelligence chip. [xiv] As of December 31st, 2023, we own a small amount of Nvidia in our dynamic and strategic balanced and growth models [xv] via our iShares Semiconductor ETF SOXX holding.
We are very cautious regarding NVDA, the company has experienced two large losses in the past five years. In the fourth quarter of 2018, NVDA stock suffered a -56% drawdown in 82 days [xvi] due to the company warning about excess inventory of graphic chips for gaming. [xvii] In 2022, NVDA stock suffered a -66% drawdown in 329 days [xviii] as cancelled orders from personal computer makers and weakness in crypto mining orders negatively impacted sales and earnings. [xix]
So, what is your benchmark, an individual stock like Nvidia that fell -66% in 329 days in 2022, or an index like the S&P 500 that fell -49% from its peak on March 27, 2000, to its low On October 9, 2022?
We counsel investors to understand what they are invested in – typically a diversified portfolio – and measure their results with the appropriate diversified, blended benchmark. Life is too short to be frustrated.
If you are not a client, we are happy to review how much risk that you are taking to achieve your returns. Please reach out to Brian Lasher (blasher@cigcapitaladvisors.com), Eric T. Pratt (epratt@cigcapitaladvisors.com) or the rest of the CIG team.
This report was prepared by CIG Asset Management and reflects the current opinion of the authors. It is based upon sources and data believed to be accurate and reliable. Opinions and forward-looking statements expressed are subject to change without notice. This information does not constitute a solicitation or an offer to buy or sell any security.
[i] calculated by CIG using data from finance.yahoo.com
[ii] Calculated by CIG Asset Management using data from finance.yahoo.com
[iii] The Daily Spark, published by Apollo 10/18/2023
[iv] Calculated by CIG Asset Management using data from finance.yahoo.com
[v] https://www.lseg.com/en/ftse-russell/indices/russell-us
[vi] https://www.msci.com/documents/10199/86494e1f-914e-4aa5-82a9-2e29ed5adbbf
[vii] https://www.investopedia.com/terms/l/lehmanaggregatebondindex.asp
[viii] The Magnificent 7 is a term coined by Bank of America analyst Michael Hartnett. The seven stocks are Alphabet, Amazon, Apple, Meta Platforms, Microsoft, Nvidia and Tesla. Calculated by CIG Asset Management as of 01/02/2024 using data from State Street Global Advisors and iShares. The S&P 500 index is represented by the SPDR S&P 500 Trust and the Russell 3000 index is represented by the iShares Russell 3000 ETF.
[ix] Calculated by CIG Asset Management using data from finance.yahoo.com
[x] Calculated by CIG Asset Management using data from Zephyr and Tamarac.
[xi] Calculated by CIG Asset Management using data from Tamarac and Zephyr
[xii] The Balanced Benchmark is a blend of 45% Russell 3000, 10% MSCI All-Country World ex US and 45% Bloomberg US Aggregate Bond indices.
[xiii] Calculated by CIG Asset Management using data from Zephyr and Tamarac
[xiv] CFRA research report dated December 8, 2023.
[xv] CIG Dynamic Growth Strategy, CIG Dynamic Balanced Strategy, CIG Strategic Growth Strategy, CIG Strategic Balanced Strategy.
[xvi] Calculated by CIG Asset Management using data from barchart.com
[xvii] https://www.cnbc.com/2018/11/16/nvidia-stock-falls-on-revenue-and-guidance-miss.html
[xviii] Calculated by CIG Asset Management using data from barchart.com
[xix] https://finance.yahoo.com/news/nvidia-stock-dropped-11-rough-231731668.html
agreement
Image: Canva

Find Your Optimal Staffing Level
If your practice has too few staff members, patient care may suffer and collections may slow down. If you have too many, you’ll face rising operational costs. Is there an optimal level that will allow you to operate your practice efficiently without letting your costs get out of control and creating dissatisfaction among patients?
Start by using medical industry benchmarks for comparison. Various organizations collect a wide variety of data on staffing levels. You’ll want to compare apples to apples, so it’s important that you use data from practices similar to yours in terms of practice area(s), size, annual revenues, and the number of physicians employed. It’s also important to follow the same methods used in the survey when determining your practice’s numbers for comparison.
Look at These Key Benchmarks
Two benchmarks you should look at are the average number of support staff per full-time-equivalent (FTE) physician and the percentage of gross practice revenue used for support staff salaries. The first benchmark is the number of full-time staff (not including mid-level providers) required to support one full-time physician. The percentage of gross revenue is total staff salary expense divided by gross revenue over the same period.
Be Ready To Adjust
If your physicians see more or fewer patients daily than the average patient load, you’ll likely want to compensate for that difference when you compare your practice with benchmarks. Looking at the number of patient visits per year or week or the gross charges per physician can help you gauge your support staff to FTE physician ratio. Similarly, your practice may require more support staff than a benchmark indicates if your ratio of mid-level providers to physicians is higher than a benchmark survey suggests. By the same token, your need for support staff may be lower if you have no mid-level providers.
Start by using medical industry benchmarks for comparison.
We Can Help
To schedule a complimentary consultation with a CIG Capital Advisors professional, click here.
Article Links:
https://www.medicaleconomics.com/view/making-medicine-better-for-women
https://insidexpress.com/lifestyle/health/the-only-guide-that-make-hiring-for-your-private-medical-practice-easy/
https://www.ama-assn.org/practice-management/private-practices/tips-help-private-practices-lessen-sting-staffing-shortages
images: iStock by Getty Images

Practice Resolutions for the New Year
The end of the year is a time for reflection. It’s also a chance to apply the lessons of the past going forward. If one of your 2022 goals is to improve the operational, administrative, and financial aspects of your medical practice, here are some ideas you might be able to incorporate in your list of New Year’s resolutions.
Review Current Patient Service Approaches
The delivery of superior patient service takes leadership and commitment to patient needs. You can resolve to use staff meetings and personal example in the coming year to reinforce your practice’s values concerning patient treatment and care.
Superior care translates into high rates of patient satisfaction. Patient surveys have been found to be a particularly effective tool in providing feedback regarding a wide range of patient care and customer service issues.
Monitor Financial Performance Regularly
Tracking your practice’s financial results during the year allows you to identify trends and make changes as needed.
You may want to put a dedicated staff member in charge of focusing on several key indicators or metrics, such as your practice’s collection rate, overhead percentage, and number of office visits. These indicators should be reviewed at regular intervals as the year progresses.
We can help you interpret what the numbers are saying and see the big picture. Staying on top of performance throughout the year can enhance your practice’s financial management.
Improve Collections and Billing
Finding a way to streamline and simplify payment for services rendered may be a goal for your practice in the coming year. One approach that can work to reduce both billing expenses and collection difficulties: Have your receptionist ask for copays before your patients leave your office – or even better, when they arrive.
Ensuring that you bill for all of your hospital services in the coming year is another worthwhile resolution. When you are seeing patients at a hospital, be sure to make a record of your work promptly and transmit the information to your billing staff. Though it’s more efficient to call your billing office immediately after you complete procedures, if that’s not feasible, create electronic or written notes for later use by your billing staff.
Establish a process for following up on unpaid accounts. Make follow-up calls within a certain number of days of when services were provided or when the original bill was due.
Establish a Training Plan
Staff training can pay off in increased productivity, improved morale, and a more efficient operation. Look into what ways your support and administrative staff could benefit from training, seminars, and other educational opportunities. Budget for a specific dollar amount to be spent on staff development each year. Online seminars and training sessions can be a cost-effective alternative.
Plan for Capital Expenditures
As you prepare your budget, identify the equipment you intend to replace and set priorities for the systems and technologies your practice will need going forward. Determine what, if any, areas in your current facility need to be remodeled or expanded.
Preparing a detailed plan with a very specific timetable for achieving goals can help you clarify what needs to be done to keep your practice competitive.
We can help identify and prioritize the measures that will help your practice run more efficiently in the coming year. Please contact us for assistance.
Finding a way to streamline and simplify payment for services rendered may be a goal for your practice in the coming year.
To schedule a complimentary consultation with a CIG Capital Advisors professional, click here.images: iStock by Getty Images

Easing into Retirement
Given the physical and emotional demands of their profession, it’s little wonder that some physicians look forward to retirement. However, many other doctors nearing retirement age are reluctant to turn their backs completely on their profession and would rather find a way to ease into retirement.
What should you do if retirement is on the horizon, but you would prefer to transition gradually into retirement by working part-time? Here are some things to consider if you are thinking of cutting back on your work hours.
Review Your Finances
First off, determine if you can afford the reduction in earnings that reducing your work hours will entail. Pay particular attention to any debt you are carrying (mortgages, etc.). Ideally, you don’t want to be overly burdened with debt once you are no longer practicing full-time.
A review of your current net worth can give you a clearer picture of your overall financial standing. Net worth takes into account the value of all your assets as well as your outstanding liabilities.
If you’ve been funding a tax-favored retirement plan, hopefully you have accumulated sufficient assets to provide a steady stream of income for all the years you may be retired. If you still haven’t met your goal, you’ll want to determine if your earnings from part-time work will allow you to comfortably continue adding contributions to your retirement plan. You’ll also want to determine when you can start taking penalty-free withdrawals from your plan(s) and project what your tax situation will look like. These are all issues we can help you assess.
Look at Your Options
If you are part of a multi-physician practice, talk to your colleagues about what arrangements can be made for you to start cutting back your hours. You may need to revise your practice agreement to incorporate a new compensation arrangement. Typically, such arrangements are based on the productivity of the part-time physician less a share of practice overhead expenses.
If you are a solo practitioner, you may find it hard to practice part-time without creating problems with your current patient base. Patients may feel that you can’t deliver the type of patient care they expect if you are practicing part-time. Bringing in a physician assistant may be helpful. However, recruiting another physician who would eventually take over the practice may be the most effective route for solo practitioners.
Give careful consideration to the financial arrangements you make with the new physician. When it comes time to sell, you’ll want to have a formal purchase agreement that outlines all of the rights, obligations, and responsibilities of the buyer(s) and the seller. It should also include a valuation of the practice.
Consider Malpractice Insurance
Don’t ignore the issue of malpractice insurance when you are weighing the pros and cons of going part-time. You need to be certain you will be covered during your part-time years and after you stop practicing completely. “Tail coverage” can protect you against any malpractice claims that may be filed against you after you retire.
We Can Help with Retirement Planning
Whether you are serious about transitioning to part-time work or are simply exploring your options, be sure to consult with us. We can help you run the numbers and evaluate your financial preparedness for retirement.
If you are part of a multi-physician practice, talk to your colleagues about what arrangements can be made for you to start cutting back your hours.
To schedule a complimentary consultation with a CIG Capital Advisors professional, click here.
images: iStock by Getty Images

Exiting Your Practice? Important Issues to Consider
Providers exit their practices for a variety of reasons — dissatisfaction with the demands of running a business, the desire for a less strenuous work schedule, frustration with insurers, retirement. If you are thinking about exiting your practice, there are several steps you should take now that will help you maximize the purchase price and ensure a relatively smooth transaction.
Lay the Groundwork
Start by taking a critical look at your practice’s current financial condition. Identify areas of weakness. For example, does your practice experience poor collections or weak cash flow? How do your staffing levels compare to those of similar practices? Issues such as these can reduce the appeal of your practice. It’s to your benefit to deal with them well before you put your practice on the market.
You’ll want to have a realistic appraisal of your practice’s potential worth before you put it up for sale. Tangible assets, such as health care equipment, computers, and furniture, are relatively easy to value, though they generally make up only a small part of a health care practice’s total value. Goodwill is an intangible asset that can be difficult to value. But there are methods that can be used to establish a reasonable estimate. Some other widely used methods include the discounted cash flows and market multiples methods.
Identify Potential Buyers
You may receive an unsolicited offer. If you don’t, consider reaching out locally or contacting a broker who specializes in exiting health care practices. An experienced broker can identify and contact qualified potential buyers.
The speed with which a sale may occur will largely depend on the deal you’re seeking. Do you want a buy-out that will let you continue to practice as an employee? In that case, looking for a group practice, hospital, or other corporate buyer may be the best route. If the sale goes through to one of these entities, you will be able to continue to work in health care without the responsibilities of ownership.
If retirement is your goal, you may opt for a gradual buy-in by a provider who will take over your practice. Typically, this arrangement requires you to employ the prospective buyer and, under the terms of the deal, after a trial period of a year or two, offer a partnership with a documented exit arrangement for you. This arrangement could be in the form of a severance package.
Review All Offers Carefully
If you receive an offer, your focus should be on the would-be buyer’s financial condition and the payment terms if you plan on retiring. If you plan to continue working at the practice with the individual or entity who may buy it, you should carefully review all ramifications, including transfer expenses and malpractice terms involved in the sale.
Apart from satisfying yourself about the financial and legal issues involved in the sale, you should also feel that you will be able to fit into the potential buyer’s organization and that your advice and input will be welcomed.
Remember, whatever way your practice’s sale is structured, there will be tax implications. Let us help you secure the most tax-advantageous sale terms. Please contact us if you would like assistance.
The speed with which a sale may occur will largely depend on the deal you’re seeking.
We Can Help
To schedule a complimentary consultation with a CIG Capital Advisors professional, click here.
Dental tools photo: Succo/Pixabay
Stethoscope photo: Julio César Velásquez Mejía/Pixabay

Maximize Revenues and Trim Expenses by Streamlining Practice Operations
Improving operational efficiencies should be an ongoing process for all medical practices. Reevaluating and examining existing procedures can help identify areas of weakness that can drain revenues and increase costs, lowering the bottom line. The following suggestions may help jump-start your own thoughts about ways you can maximize your practice’s revenue stream and reduce costs without sacrificing patient care.
Keep Coding Current
Miscoding is expensive: It can reduce reimbursements and cause delays or denied claims. Miscodes are often due to old data, under coding to avoid penalty risk, or leaving coding decisions to inexperienced support staff.
For more accurate coding, maintain updated coding manuals and software, keep a code reference summary handy in exam rooms, and use online coding resources. If you make notes during each patient visit, you’ll be able to bill more accurately. Taking coding refresher courses will help your staff stay current with coding practices.
Finally, periodic assessments of your practice’s coding accuracy can help uncover problem areas. These assessments could include a review of your practice’s forms and a comparison of billing codes with the actual services that were provided.
Improve Employee Productivity
Consider these ideas for improving productivity:
-
-
- Set productivity goals and offer incentives to your staff for reaching those goals
- Delegate administrative functions (ensure that physicians spend most of their day doing only what physicians can do)
- Plan patient flow so that physician and medical assistant billable time is maximized
-
Exercise More Efficient Control over Staff Time
It is often possible to trim overtime expenses without reducing the quality of patient care. Start by reviewing the payroll records of your non-exempt employees to determine who worked overtime and why. Find out if your practice was fully staffed and simply busy or if it was short one or more employees on the days when the overtime occurred. If overtime was necessary because you were short-staffed, see if this was due to vacations or some other controllable situation. It may be time to revise your practice’s policy on vacation time if scheduled time off was the cause of the jump in overtime.
Update Fee Schedules
Patients can be price conscious and resistant to fee increases. Nevertheless, if your practice hasn’t raised fees in some time, you may want to consider appropriate increases. In addition, you should periodically examine the reimbursement rates of all the plans you participate with and reevaluate whether it makes economic sense to continue accepting patients from some of the ones that reimburse poorly.
Improve Your Purchasing Practices
Medical and office supplies can be a significant part of a practice’s expenses. Busy practices may take the path of least resistance and continue ordering from the vendors that have always supplied them. That can be an expensive mistake. Choose several of your practice’s “high-volume” items and find out how much other vendors are charging. Use that information to negotiate lower prices with your current suppliers, consolidate orders with fewer vendors, or switch to new suppliers to save money.
We Can Help
We can help you identify areas where streamlining operations may help optimize your practice’s bottom line. Please call.
. . . if your practice hasn’t raised fees in some time, you may want to consider appropriate increases.
To schedule a complimentary consultation with a CIG Capital Advisors professional, click here.
Photo: Daniel Sone/Unsplash

Measure Your Medical Practice’s Performance
Is your medical practice moving forward, standing still, or
losing ground? You’ll know the answer if you compare
different aspects of your practice’s operations to appropriate benchmarks
(as you can do here
using the CIG Capital Advisors Medical
Practice Dashboard). Benchmarking can give you the data you need to make
informed management decisions about the direction of your practice.
What To Measure
There are two types of benchmarking: Performance and
process. Performance benchmarking compares a practice’s operating performance
internally over time and externally against other practices of a similar size
in the same specialty. Process benchmarking compares a practice’s work
protocols. By tracking key benchmarks from quarter-to-quarter or year-to-year,
you can identify the areas in which progress is being made.
Start by choosing a few indicators that are important to
you. For each indicator, determine your objective and define what you’ll
measure and how you’ll do it. Keep tracking the data regularly so that you can
make meaningful comparisons over time. Here are some of the indicators your
practice may want to use in its analysis.
Profitability/Cost Management
Look at measures such as net income (or loss) per full-time
equivalent physician and operating cost per physician. Other useful areas to
analyze would include operating costs as a percentage of total medical revenue
and total support staff cost per physician.
Billings and Collections
What percentage of submitted claims is rejected by
third-party payers? Is that percentage higher or lower than it has been in the
past? If you determine that the number is increasing, you’ll need to review the
quality of your coding. If coding errors are at fault, it’s critical that you
tackle this issue immediately.
Examine the percentage of accounts receivable over 120 days.
Is it higher or lower than what has been your experience? What about your
practice’s fee for service collection percentage or the dollar amount of bad
debts per physician? These are measures that you can evaluate.
If you track your copay collection rate for several quarters
and see that it is deteriorating, have your front desk staff pull up each
patients’ records when making appointments and remind them about past due
payments. In addition, remind your front desk employees to ask for copays at
the time of service and to request any outstanding amounts.
Patient No-shows
If your measurement of patient no- shows reveals an uptick
in the numbers, consider having your staff make reminder calls or charging for
missed appointments.
Time Patient Spends in Office
Patients resent lengthy waiting times. You can track the
average time patients spend waiting to see a physician or physician’s
assistant. Start by giving a percentage of patients (10%, for example) a card
that your receptionist time stamps on arrival and collects and stamps again on
departure. If the data reveal an increase in wait times, overbooking may be an
issue. If that’s the case, you’ll want to reexamine your procedures and time
blocking. You may even have to look into adding another physician, physician’s
assistant, or nurse practitioner.
There are other indicators your practice can use to evaluate
how well it is doing. Keep tracking the data regularly so that you can make
meaningful comparisons over time, and be sure to try our Medical
Practice Dashboard to see how your medical practice compares to other peer
practices nationally. For a confidential consultation with a CIG Capital Advisors
medical practice advisor, email Brian Lasher.

Optimizing Your Healthcare Practice’s Income
Enhancing revenue and controlling expenses should be a financial focus of every medical practice. Improving operational efficiencies can help bring a practice closer to optimal performance. Here are some ways you can maximize your medical or dental practice’s revenue stream and reduce costs without sacrificing patient care.
Keep Coding Current
Coding errors are all too common. Simple errors can end up costing medical practices money as well as time to rectify mistakes. Delays or denied claims may translate into reduced reimbursements, which, in turn, affect cash flow.
To minimize coding errors, you need to identify the cause of the problem. Typically, miscodes are due to under-coding to avoid penalty risk, using outdated data, or leaving coding decisions to inexperienced support staff. Periodic assessments of your practice’s coding accuracy can help uncover problem areas. These assessments could include a review of your practice’s forms and a comparison of billing codes with the actual services that were provided.
Maintaining updated coding manuals and software, keeping a code reference summary handy in exam rooms, and using online coding resources can help your practice attain a more accurate coding rate. So too will making notes during each patient visit. Be sure to have your staff attend refresher courses to help them stay current with coding practices.
Improve Employee Productivity
Eliminating inefficiencies and boosting employee productivity can directly benefit your practice’s bottom line. Try these approaches to improving the productivity of your practice:
- Define productivity goals and offer incentives to your staff for reaching those goals.
- Delegate administrative functions so that physicians spend the greater part of their day seeing patients.
- Maximize physician and medical assistant billable time by planning patient flow carefully.
Better Control of Staff Time
Are your overtime expenses increasing from quarter to quarter? While some overtime is unavoidable, a consistent rise in overtime hours deserves some scrutiny. Review the payroll records of your non-exempt employees to determine who worked overtime and why. Was your practice fully staffed and simply busy or was it short one or more employees on the days when the overtime occurred? If overtime was necessary because you were short-staffed, see if this was due to vacations or some other controllable situation. It may be time to revise your practice’s policy on vacation time if scheduled time off was the cause of the overtime.
Update Fee Schedules
If your practice hasn’t raised fees in some time, you may want to consider appropriate increases. Just be aware that some patients may be resistant to fee increases and could switch to another provider. In addition, take a look at the reimbursement rates of all the plans you participate in. Run the numbers to determine whether it makes financial sense to continue accepting patients from some of the plans that reimburse poorly.
Buy Smarter
Medical and office supplies make up a portion of a practice’s expenses. Yet, some practices rarely shop around for more competitive prices. You can control expenses by becoming a smarter shopper. Pick some of your practice’s “high-volume” items and find out how much other vendors are charging. Use that information to negotiate lower prices with your current suppliers, consolidate orders with fewer vendors, or switch to new suppliers to save money.
We Can Help
We can work with you to identify areas in your practice where streamlining operations may help optimize your healthcare practice’s bottom line. For a confidential consultation with a CIG Capital Advisors medical practice advisor, email Brian Lasher.

Examine Your Healthcare Practice’s Cash Flow to Keep Business Healthier
Medical or dental practice expenses have to be paid — whether cash flow is strong or weak. Focusing on cash inflows and outflows can help ensure that your practice will have enough cash available to meet its ongoing needs.
Examine Cash Inflows
How long does it take to convert a patient visit or a medical procedure into cash in the bank? Because receiving payment for services in a timely fashion is a critical element in effective cash management, you want to be sure every charge is accounted for, recorded, and submitted for payment promptly.
Survey your past due accounts and identify where delays have occurred in receiving payment from insurers and patients. There may be places where you can tighten procedures to minimize the likelihood of payment delays.
For example, coding errors are the source of many denied claims. By training staff to focus on accuracy in coding, your practice should reduce the number of incorrect claims that have to be resubmitted to insurers. Consider setting time goals for your staff to submit clean claims after a service is rendered, and base bonus payments on your staff reaching these goals.
Have your staff check patients’ insurance coverage every time they have an appointment to ensure that you have the most up-to-date information. If insurer information is not constantly updated and verified, you could end up submitting claims to an insurer that no longer covers the patient.
Your practice should have a system for generating up-to-date information on the status of each outstanding account. These reports should include the date each bill was sent, the current balance, and the number of days delinquent. Your staff can use that information to contact delinquent patients on a predetermined schedule.
Finally, whenever possible, have your front desk staff collect patient copays, deductibles, and prepays at the time of service. You can make paying up front easier for patients by accepting debit and credit card — and possibly even online — payments.
Track Cash Outflows
Paying bills as soon as they are received may not be the most effective way for your practice to manage cash flow. An automated accounts payable system that organizes your payments by due date is preferable. However, if a vendor offers your practice a discount for early payment, you will need to take that factor into account. Rent, utilities, and key suppliers should be paid before your practice pays bills with more flexible terms.
Consider renegotiating vendor contracts. You may be able to negotiate with certain vendors for longer payment terms — extending payment terms from, for example, 30 days to 60 days is equal to receiving an interest-free loan. Schedule a meeting with key vendors at least yearly to identify where they may have some flexibility in reducing their charges for supplies or services. You can always look for alternative vendors if your current ones seem unwilling to bend on prices.
Finally, review other areas of your operations to see if you can reduce costs. If you have any outstanding bank loans and are in a cash flow crunch, ask to renegotiate for more favorable terms.
Cash flow is crucial to your practice’s financial health. If you have had periods in the past when cash flow has been tight, take a look at what created the issue. We can help you review your current cash-management practices and suggest potential improvements. To schedule a complimentary consultation with a CIG Capital Advisors professional, click here.

Expanding your medical or dental practice to offer telehealth patient care
Telehealth (also called telemedicine) is the use of information and telecommunications technologies to provide health care across time and/or distance1, and its use has become more prevalent during the 2020 coronavirus pandemic. The two-way, real time interactive communication between a patient and a practitioner at a distant site through telecommunications equipment that includes, at a minimum, audio and visual equipment 2 can be done on one of four main telehealth platforms: live video, store and forward, remote patient monitoring and mHealth.
One of the early benefits of telehealth was its ability to provide rural communities with practitioner access even if the patient couldn’t be physically present. Given the COVID-19 crisis, the use of telehealth as a means to adhere to stay-at-home and social distancing laws has also garnered greater attention.
The Centers for Medicare & Medicaid Services have significantly expanded access to telehealth services for Medicare beneficiaries.3 The majority of these regulation changes are temporary and effective during the public health emergency, but Medicare will now pay for telehealth services at the same rate as regular, in-person visits and include the patient’s home as a telehealth site.3 The department of Human and Health Services (HHS) Office of Civil Rights has announced that it will waive HIPAA violations against providers acting in good faith to serve patients through everyday communication technologies, such as FaceTime or Skype. This allows the use of smartphones; however, the encounter may not be conducted over a public platform, such as Facebook Live.4 Further, providers can use telemedicine to prescribe controlled substances without a prior medical evaluation.5
Currently, licensure requirements are waived to allow providers to virtually treat patients in other states, increasing telehealth opportunities.6 In addition, practitioners will not be subject to any waivers or sanctions for reducing cost-sharing obligations. HHS will not conduct audits to ensure that a prior relationship existed between a patient and practitioner for telehealth visits.3
Please note that telehealth laws may differ from state to state, and commercial insurance carrier policies may differ from policy to policy.
There are many ways patients and practitioners can benefit from incorporating telehealth into a care plan. Telehealth allows providers to free up space in waiting rooms, expand catchment areas and reduce overhead expenses. Done right, it can also serve to improve patient accessibility and convenience as well as eliminate transportation expenses for regular checkups.
For providers who decide to pursue telehealth, be aware that there are many different platforms to choose from. Remember to reach out to the patient network so they are aware of the practice’s telehealth capabilities, and be sure to highlight the service on the practice website.
A professional at CIG Capital Advisors can help you with telehealth planning, such as choosing the right telehealth platform and marketing strategy. For a confidential consultation with a CIG Capital Advisors medical practice advisor, email Brian Lasher.
Sources
- https://effectivehealthcare.ahrq.gov/products/telehealth-acute-chronic/research-protocol
- https://www.medicaid.gov/medicaid/benefits/telemedicine/index.html
- https://www.cms.gov/newsroom/fact-sheets/medicare-telemedicine-health-care-provider-fact-sheet
- https://www.hhs.gov/about/news/2020/03/17/ocr-announces-notification-of-enforcement-discretion-for-telehealth-remote-communications-during-the-covid-19.html
- https://www.dea.gov/press-releases/2020/03/20/deas-response-covid-19
- https://www.cms.gov/files/document/covid-19-physicians-and-practitioners.pdf
